|
Abstract
Objectives: The
aim of this study was to evaluate the attitudes,
knowledge and perception of medical students about
elderly patients before and after implementation
of a new geriatrics curriculum and to assess perceived
attainment of objectives in geriatric module.
Methods: This
was a pre-post cohort study of seventy 6th year
(first clinical year) medical students. Questionnaires
were provided prior and post geriatric assessment.
Utilization of common geriatric tools was taught
in a tutorial and then reinforced in small group
(case based) discussions. Questionnaire was mainly
comprised of pre and post questions, perception
of students regarding geriatric care and students'
perceived attainment of objectives from geriatric
module. Statistical analysis was performed using
SPSS 20.v. Data were expressed in frequencies,
mean and percentages. Paired t test was used to
evaluate the significant difference between pre
and post responses.
Results: A total
of 70 students participated in the study. 14.3%
were male and 85.7% were female students with
mean age of 22.84 ± 1.03. The mean scale
score for students' basic understanding of geriatrics
was significantly higher after completion of education
program compared with scores prior to training
(p < 0.001, 95% CI: 3.01-4.87) with an increase
of 3.943 in the mean scale score. In the same
way the mean scale score of students' knowledge
of geriatrics was statistically higher after completion
of education program compared with scores prior
to training (p < 0.001, 95% CI: 3.13-4.5) with
an increase of 3.829 in the mean scale score.
Overall students' feedback about geriatric module
at the end of rotation was good as more than two
third clumped from achieved to outstandingly achieved.
Conclusion: Medical
students who received education during their module
showed improvement in levels of knowledge about
geriatrics.
Key words: Geriatrics,
Curriculum, Feedback, Education, medical students
|
- - - - - - - - - - - - - - - - - - -
- - - - - - - - - - - - - - - - - - - - - - - -
Background
Geriatrics refers to the clinical aspects of aging and
the comprehensive health care of older persons. Evidence
from several studies and national surveys indicates
that families are the major care providers for impaired
older adults. As fertility rates decline, the proportion
of persons aged 60 and over is expected to double between
2007 and 2050. A survey of US medical schools showed
that 71% percent of schools either had geriatrics as
a medical student clerkship or as part of a required
clinical rotation [1-2]. Ageing is characterized by
progressive and heterogeneous decline in physiological
reserve of all organ systems. There are an estimated
101,145 60-plus people in Oman, representing 5.2 per
cent of its population. Five per cent of these are bed-ridden
[3-4].
Every elderly person has unique and specific needs.
Ministry of Health (MOH) Oman runs a comprehensive assessment
program to determine the immediate needs of an individual.
This defines whether the person needs health or social
intervention or both. Globally the number of elderly
is expected to increase three-fold by 2050 [5]. This
rise of the aging population has had an impact on the
practice of medicine, as the unique needs of the elderly
require the presence of a multidisciplinary and comprehensive
medical approach [6]. The need for geriatric education
has been repeatedly cited in the United States where,
according to one study, every third patient seen by
a medical student is elderly [7]. Teaching geriatrics
in medical schools leads to improvement in geriatric
knowledge, skills and attitudes of undergraduate medical
students [8].
Evaluation and treatment of elderly patients requires
specific knowledge, attitudes, and skills that are acquired
across the continuum of medical education. Development
and implementation of new geriatrics experiences has
been undertaken throughout the medical school and residency
curriculum [9]. Geriatric/Palliative care education
in the undergraduate medical curriculum found considerable
evidence that current training is inadequate in dealing
with end of life issues, most strikingly in the clinical
years. Reforming existing health care curriculum to
incorporate palliative care education is often faced
by many challenges on a number of levels [10]. There
is a strong need to incorporate geriatric palliative
care education into primary health care education such
that there is an overlap between primary health care
and palliative care. The attitudes and competencies
required to provide high-quality care overlap substantially
with those required to provide excellent primary care
[11-12].
To strengthen and make it more effective in terms of
teaching and experiential learning of geriatric /palliative
care in family medicine few steps are already being
done. Thus, a process of needs assessment, identifying
gaps in knowledge, consultations with the curricula
reformers and strategic planning is thought to be an
effective catalyst for curricular change [13-14]. Geriatric
care is an integral part of teaching and learning in
family medicine. Caring for patients with a chronic
or terminal illness is an opportunity to use knowledge
and skills as part of a team and to give patients the
time and the opportunity to discuss some of their deepest
fears and anxieties. Cure may not always be a possibility
but empathy and care will always be required, and the
doctors of the future need to be aware of this.
Goals of family medicine program are to have a competent
clinician in respect of diagnosis and providing evidence-based
cost-effective management of conditions commonly met
at the primary health care level. The purpose of this
study was to evaluate the attitudes, knowledge and perception
of medical students about elderly patients before and
after implementation of a new geriatrics curriculum
and to assess perceived attainment of objectives in
geriatric module.
Methods
A favorable ethical opinion was obtained from the Oman
Medical College ethics committee at the beginning of
study.
Curricular Design
A detailed study of curriculum design and planning was
then undertaken. The student-centered, problem-based,
integrated model seemed most applicable in our setting
and was adopted. Key topics were identified through
an overview of American Association of Medical Colleges'
list of common geriatric competencies. We integrated
a geriatric course into an existing curriculum and described
the necessary steps required to implement it. The overall
aim was to introduce a geriatrics education program
within the existing curriculum [13-15].
The course content was reviewed by experts, course coordinators
and academic vice dean. Exit level and specific enabling
objectives of the geriatric program were made. Teaching/learning
strategies were devised and consisted of small group
tutorial sessions, case based scenarios, role play,
simulated history taking and a few large class format
sessions.
Curricular Implementation
Teaching/learning strategies were devised and consisted
of small group sessions. The new module was incorporated
in the existing eight week family medicine rotation
in year 6 which is the first clinical year. In all,
five groups of students rotate through family medicine
for eight weeks through the year, with this class having
a total of 70 students. The geriatric course objectives
for this year were to familiarize students with history
taking and physical examination and use of common geriatric
assessment tools in elderly patients. In addition basic
knowledge of aging physiology and pharmacology were
also incorporated in this rotation.
Prior to the introduction of geriatrics in the family
medicine rotation, faculty development initiative was
taken. Family medicine faculty underwent a basic two
hour training session on teaching a problem based geriatric
history and physical examination method. Besides this
reading materials were provided as additional learning
resources.
For students, two tutorial sessions were conducted to
cover the basics of aging physiology and pharmacology
and small group sessions in which problem based scenarios
were used to practice history-taking in the context
of aging physiology and pharmacology. Geriatric assessment
and use of common geriatric tools was taught in a tutorial
and then reinforced in small group case
based discussions. Each student rotates to geriatric
clinic in a government primary care clinic and had opportunity
to assess patients. Opportunistic learning in terms
of history taking and geriatric assessment was also
provided to students in their clinical sessions during
encounters with elderly patients throughout their eight
week rotation.
Learning Outcomes and
Core Competencies in Geriatric Module
o Acquire knowledge of the demography and epidemiology
of ageing;
o Recognize the scientific basis of geriatric medicine
and the differences in medical care of older patients;
o Develop foundational competencies in performing important
aspects of a geriatric assessment;
o Recognize and appreciate physiologic diversity and
its clinical significance in elderly patients;
o Establish the interactions between medical diagnoses,
functional impairment, and medications;
o Interact with patients and their caregivers using
a bio-psychosocial approach;
o Develop a clear understanding of important basic ethical
principles governing care of elderly patient;
o Explore healthcare services for the elderly and healthcare
financing for the elderly with specific reference to
Oman.
List of Teaching Methodologies and Topics in Geriatric
Module
Small Group Interactive Workshops/Tutorials
o Approach to the older person and Principles of geriatric
medicine
o Physiology of ageing and functional impairment
o Cognitive and behavioral issues in ageing
o Common medical problems in old age/ Prevention, rehabilitation
and care
o Principles of geriatric pharmacology / Prescribing
in older persons
o Health promotion and disease prevention in older persons
o Nutritional needs & dental/oral hygiene
o Health care services for the elderly in Oman
Once in 8 week rotation:
visit to Elderly care center
o Clinical skills in geriatrics: history taking and
physical examination
Once in a week clinical
rotation at Geriatric clinic
o Clinical skills in geriatrics: history taking and
physical examination
o Approach to geriatric patients' problems in primary
care
Curriculum Evaluation
Student's feedback on this curriculum was taken to further
refine the curricular content and strategies as necessary.
Two study instruments were used to assess the course.
Student knowledge was assessed via a single best option
test which was given to all students as a pre-test prior
to the introduction to geriatrics. The UCLA geriatric
knowledge test, a validated questionnaire used in previous
studies, was reviewed for pre-test development. Keeping
in line with the overall objectives of history taking
and assessment skills for students, a modified pretest
was designed. The questionnaire consisted of questions
on aging demographics, aging physiology (cardiovascular
and central nervous system), aging pharmacology, history
taking, nutritional, functional, and gait assessment.
The same questions were given (in a different order)
to the students at the end of the geriatric sessions
as a post test. Scores were reported as the total number
of correct responses.
Attitudes toward geriatrics were measured using a geriatric
attitude questionnaire adapted from the 14-item UCLA
Geriatrics Attitudes Scale [16]. The scale was designed
to assess general impressions about older people, perceived
value of older people, distributive justice of societal
resources toward older people, attitudes toward caring
for older patients, perceived potential benefits of
treating older patients, and personal economic concerns
about caring for older patients. The additional two
questions were used to assess attitudes toward working
with elders and to evaluate attitudes regarding elders'
perceived level of trust in discussing sensitive issues
with medical providers. A self-administered evaluation
form was also distributed at the end of the rotation
to all students. The overall quality of teaching was
included in the feedback form and a global rating for
the overall module was also assessed. At the end of
the rotation all students were asked to fill in the
feedback form. This form consisted of nine questions
related to the course objectives rated on a forced choice
format (a variant of the Likert scale) questionnaire
with five choices ranging from 1 ('not achieved') to
5 ('outstandingly achieved'). Space was also provided
at the end of the form for additional comments. Student
name on the course evaluation form was optional. No
extra resources or funds were used.
Statistical Analysis
Statistical analysis was performed using SPSS (IBM SPSS
Statistics 20.0). Data were expressed in frequencies,
mean and percentages. Each participant's individual
score was calculated for pre and post question by assigning
1 for correct and 0 for the wrong response. Mean scale
scores for the pre and post questionnaire of each scale
were evaluated for significance difference using the
paired t-test for hypothesis testing.
Results
A total of 70 students participated in the study. Age
ranged from 21 to 25 years with mean of 22.84 ±
1.03. 14.3% were male and 85.7% were female students.
Table 1 shows student's pre and post-test geriatric
teaching correct responses. Significant difference was
found regarding geriatric teaching between student's
pre and post correct responses (p <0.001, 95% CI:
5.228-13.24). Similarly, significant difference was
observed between pre and post-test knowledge MCQ correct
response (p <0.001, 95% CI: 12.39-23.39). The mean
scale score for students basic understanding of geriatrics
was significantly higher after completion of education
program compared with scores prior to training (p <
0.001, 95% CI: 3.01-4.87) with an increase of 3.943
in the mean scale score. In the same way the mean scale
score of students' knowledge of geriatrics was statistically
higher after completion of education program compared
with scores prior to training (p < 0.001, 95% CI:
3.13-4.5) with an increase of 3.829 in the mean scale
score. Similarly, significant difference was found between
pre and post responses among both male and female students.
All students were also satisfied with the quality of
teaching with 90% rating it as good or higher. Most
students (89%) rated that the overall objectives were
clear and achieved. Table 3 shows the students' perceived
attainment of objectives from geriatric module at the
end of rotation.
Table 1: Student's Pre and Post-Test Geriatric Teaching
Correct Responses among 70 Students - n (%)
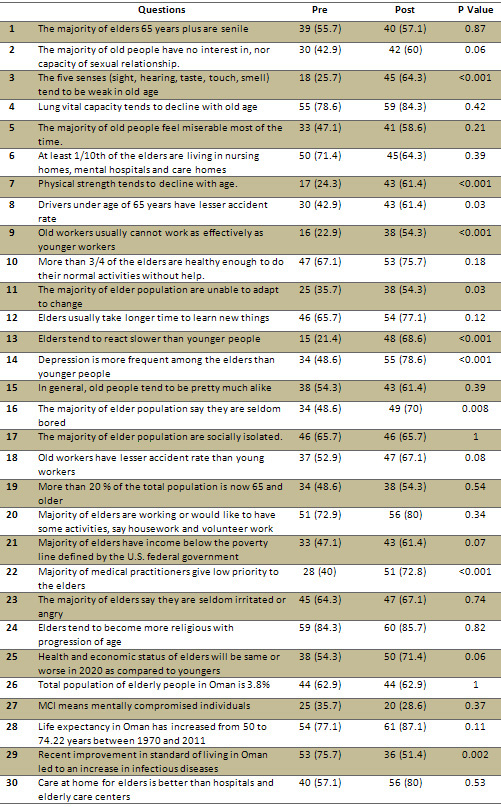
Click here for
Figure 1. Students Geriatric
Teaching Correct Pre and Post-Test Responses with significant
difference
Table 2: Pre and Post-Test
Knowledge MCQ Correct Response among 70 Students - n
(%)
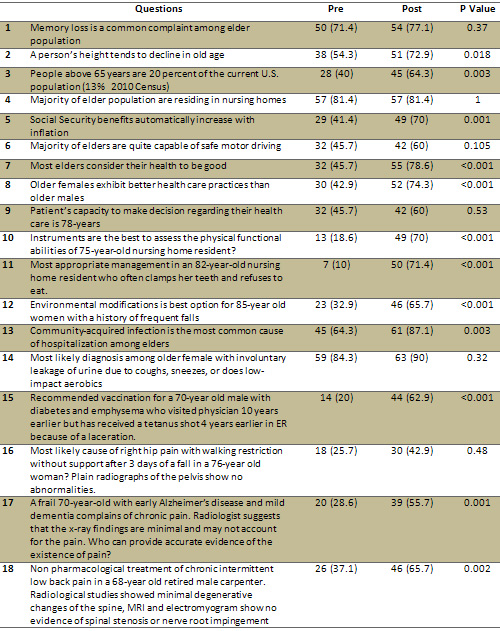
Click here for Figure
2. Students' Knowledge MCQ Correct Pre and Post-Test
Responses with significant difference
Click here for Table
3: Students' Perceived attainment of objectives from
geriatric module at the end of rotation - n (%)
Discussion
There has been a rise in the elderly population throughout
the world including Oman because of good living standards.
The unique needs of the elderly require a multidisciplinary
and comprehensive medical approach for medical care
and health promotion. This is imperative to have structured
undergraduate and postgraduate medical curriculum to
train our future doctors how to handle these population
[16].
The knowledge scores improved considerably in students
who attended the geriatrics course in their first clinical
year. This change was similar to improvement in student
scores reported in other schools where geriatrics was
introduced [17]. Effective teaching and learning methods
for geriatric competencies are mandatory to enhance
knowledge in geriatric medicine [18-19].(Table I, Figure
I) Different areas of knowledge also showed improvement;
the same finding is also reported in literature that
students were successful in fulfilling objective, which
was to bring about an improvement in students' knowledge
and attitudes in geriatrics [20].
Using pre and post rotation testing, we were able to
demonstrate significant knowledge acquisition on a variety
of topics pertaining to geriatric medicine and care
of the older patient. Various research studies have
shown the same result [21-23](Table II, Figure II).
This study'sresults have shown overall level of confidence
and competency in students and better empathic response
towards geriatric population [24-25].
Student's perception regarding geriatric care was improved
after they finished the rotation. The overall course
was well-received by students, and teaching strategies
were considered good or better by a strong majority
of students. There were a small number of students who
rated the course unsatisfactory in terms of achievement
of objectives. This was also reflected in the course
evaluation scores where students rated achievement of
objectives in teaching and learning physiology and pharmacology
slightly lower than the other areas. As reported in
literature students may have some negative attitudes
towards geriatric medicine that need to be addressed
appropriately [26-27].(Table III).
One of the important points in students' feedback was
their report of difficulty in students' ability to generate
a problem list in geriatric patients as well as using
a tool for geriatric assessment. Basic understanding
and exposure to geriatrics can develop a good and effective
curriculum for undergraduate medical students. Teaching
and learning focused on geriatric issues as well as
assessment after module will further improve the outcome
[28-29]. Increase in geriatric population in Oman needs
a focused and structured undergraduate as well as postgraduate
curriculum to train our future doctors [30].
Future research should address the issue of translating
acquired knowledge in geriatric medicine into demonstrated
clinical skills, when caring for the elder population.
Future research may involve identification of the ideal
curriculum models in geriatrics that provide support
to the students' learning and developing and validating
instruments to measure effectiveness of curricular innovations.
Conclusion
Medical students who received education during their
module showed improvement in levels of knowledge about
geriatrics. This study has demonstrated that a combined
didactic and clinical program successfully increased
students' knowledge in Geriatric Medicine. Adding a
student-based approach and strengthening assessment
are future steps towards improving this curriculum.
Changing population demographics mandate not only the
need for more specialists in geriatric medicine, but
also primary care physicians should have an adequate
knowledge of the principles of caring for older patients.
This must be accomplished with a mandatory rotation
in medical schools.
References
1. Population Division, DESA, United Nations. Chapter
II: Magnitude and speed of population ageing. In: World
Population Ageing 1950-2050. [Online]. Available at
< http://www.un.org/esa/population/publications/worldageing19502050/pdf/80chapterii.pdf
> Last Accessed Dec 2013
2. Geriatrics Lags in Age of high tech Medicine. In:
The New York Times. Oct 18, 2006
3. Sulaiman AJ, Al-Riyami A, Farid S, Ebrahim GJ. Oman
Family Health Survey 1995. J Trop Pediatr. 2001; 47(Suppl
1):1-33.
4. Jamison DT, Sandbu ME. Global Health. WHO ranking
of health system performance. Science. 2001; 293:1595-1596.
5. Lambourne A. Oman's population profile 1970-2000.
Muscat, Sultanate of Oman: Ministry of Health; 1990.
6. Van Zuilen MH, Mintzer MJ, Milanez MN et al. A competency-based
medical student curriculum targeting key geriatric syndromes.
Gerontol Geriatr Educ 2008; 28:29-45.
7. Sabzwari S, Azhar G. Ageing in Pakistan-A New Challenge.
Ageing International. Epub 26 November 2010.
8. Hughes NJ, Soiza RL, Chua M. Medical student attitudes
toward older people and willingness to consider a career
in geriatric medicine. J J Am Geriatr Soc 2008; 56:334-338.
9. McCrystle SW, Murray LM, Pinheiro SO. Designing a
learner-centered geriatrics curriculum for multilevel
medical learners. J Am Geriatr Soc 2010;58:142-151
10. Leipzig RM, Granville L, Simpson D. Keeping granny
safe on July 1: A consensus on minimum geriatrics competencies
for graduating medical students. Acad Med 2009; 84:604-610.
11. Reuben DB, Lee M, Davis JW et al. Development and
validation of a geriatrics knowledge test for primary
care residents. J Gen Intern Med 1997; 12: 450-452.
12. Cleary LM, Lesky L, Schultz HJ et al. Geriatrics
in internal medicine clerkships and residencies: Current
status and opportunities. Am J Med 2001; 111: 738-741.
13. Harden RM, Sowden S, Dunn WR. Educational strategies
in curriculum development: the SPICES model. Medical
Education. 1984; 18(4):284-297.
14. Harden RM. Ten questions to ask when planning a
course or curriculum. Medical Education. 1986; 20(4):356-365.
15. Bland CJ, Starnaman S, Wersal L, Moorehead-Rosenberg
L, Zonia S, Henry R. Curricular change in medical schools:
how to succeed. Academic Medicine. 2000; 75(6):575-594.
16. Geriatric Competencies for Medical Students. Recommendations
of the July 2007 Geriatrics Consensus Conference. Available
from http://www.aamc.org. Accessed March 2010.
17. Oates DJ, Norton LE, Russell ML. Multisite geriatrics
clerkship for fourth-year medical students: A successful
model for teaching the Association of American Medical
Colleges' core competencies. J Am Geriatr Soc 2009;
57:1917-1924.UCLA geriatric knowledge test. [Online].
Available at: <http://www.ucop.edu/agrp/docs/la_knowledge2.pdf
> Last Accessed February 20014
18. Medina-Walpole A, Clark NS, Heppard B, Dannefer
E, Hall W, McCann R. A user's guide to enhancing geriatrics
in an undergraduate medical school curriculum: the ten-step
model to winning the "geriatric game". Journal
of the American Geriatrics Society. 2004; 52(5):814-821.
19. Strano-Paul L. Effective teaching methods for geriatric
competencies. Gerontol Geriatr Educ 2011; 32:342-349.
20. Sabzwari SR, Bhanji S, Zuberi RW Integration of
Geriatrics into a Spiral Undergraduate Medical Curriculum
in Pakistan: Evaluation and Feedback of Third-Year Medical
Students .Education for Health. December 2011.24(3):622.
21. Eleazer GP, Giles V, Wieland GD. Evaluation of an
Undergraduate Medical Geriatric Curriculum through Use
of Test Question Analysis. Geriatrics & Gerontology
Education. 1998; 19(1).
22. Struck BD, Bernard MA, Teasdale TA. Effect of a
mandatory geriatric medicine clerkship on third-year
students. Journal of the American Geriatrics Society.
2005; 53(11):2007-2011.Nieman LZ, Vernon MS, Horner
RD. Designing and evaluating an episodic, problem-based
geriatric curriculum. Family Medicine. 1992; 24(5):378-381
23. Warshaw GA, Bragg EJ, Brewer DE, Meganathan K, Ho
M. The Development of Academic Geriatric Medicine: Progress
toward Preparing the Nation's Physicians to Care for
an Aging Population. Journal of the American Geriatrics
Society. 2007; 55(12):2075-2082.
24. Supiano MA, Fitzgerald JT, Hall KE, Halter JB. A
vertically integrated geriatric curriculum improves
medical student knowledge and clinical skills. Journal
of the American Geriatrics Society. 2007; 55(10):1650-1655.
25. Fitzgerald JT, Wray LA, Halter JB, Williams BC,
Supiano MA. Relating medical students' knowledge, attitudes,
and experience to an interest in geriatric medicine.
Gerontologist. 2003; 43(6):849-855.
26. Smith MR, Marcy ML, Mast TA, Ham RJ. Implementation
and evaluation of a model geriatrics curriculum. Journal
of Medical Education. 1984; 59(5):416-424.
27. Golden AG, van Zuilen MH, Mintzer MJ. A fourth-year
medical school clerkship that addressed negative attitudes
toward geriatric medicine. J Am Geriatr Soc 2010; 58:746-750.
28. Atkinson HH, Lambros A, Davis BR, Lawlor JS, Lovato
J, Sink KM, Demons JL, Lyles MF, Watkins FS, Callahan
KE, Williamson JD. Teaching medical student geriatrics
competencies in 1 week: an efficient model to teach
and document selected competencies using clinical and
community resources. J Am Geriatr Soc. 2013 Jul; 61(7):1182-7.
29. Sutin D, Rolita L, Yeboah N et al. A novel longitudinal
geriatric medical student experience: Using teaching
objective structured clinical examinations. J Am Geriatr
Soc 2011;59:1739-1743
30. Vaidya SK. State steps in to take care of elderly
in Oman. [Online]. Available at < http://gulfnews.com/news/gulf/oman/state-steps-in-to-take-care-of-elderly-in-oman-1.206123>
.
|

